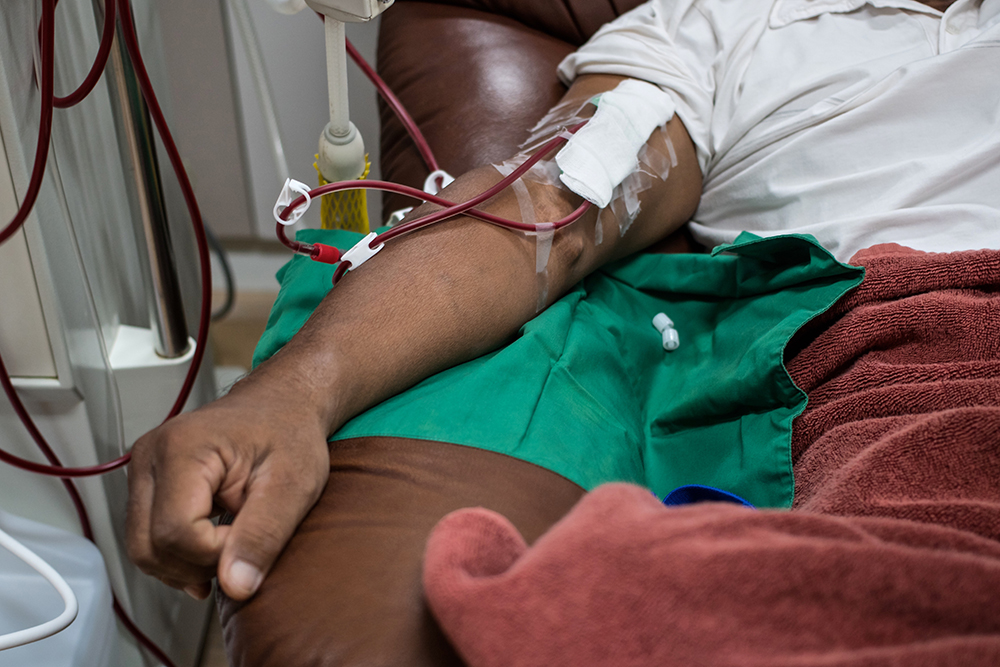
In part-1 of ‘Yarns’ from the North’, ICAN E-News caught up with Toni Cork, General Manager and Financial Counsellor at HK Training & Consultancy (HKTC), a registered training organisation, based in Darwin, NT. The team at HKTC do amazing work with the Nightcliff Renal Facility, an extremely important job given the alarming reality that 32.4% of Indigenous people in the Northern Territory are living with signs of kidney disease, the highest rate of any state or territory in Australia.
Welcome Toni!
Given your experience working within remote Indigenous communities, what connection do you see between financial hardship and health?
“Taking care of yourself is the last thing on the list for people in financial hardship. Once the essentials like rent and power are paid, there’s little left over to spend on eating healthy foods and exercising. Often fridges are old and don’t work properly, which causes food to spoil quickly, and not every household has a washing machine, which means clothing and bedding can be used for months before there’s an opportunity to wash them. Of course, this then increases the chances and spread of skin infections such as scabies, which often leads to strep infections – the number one cause of rheumatic heart disease. These circumstances, accompanied with lack of housing, limited health resources in language, and health staff who speak language, create a massive health dilemma and an increase in chronic diseases such as kidney disease.”
Can you tell me about the cost and access to healthy food in the remote communities that you service?
“There has been a marked decrease in the cost of fresh fruit and vegetables in remote communities over the last ten years. However it’s still anywhere from $1 – $5 more expensive per item than buying from a supermarket in Darwin. There’s also little or no access to dietary requirements such as milk alternatives or gluten-free pasta’s. And while healthy food has decreased in price other items such as bread, milk, cereals, cheese, spreads, tea and coffee are two to three times more expensive than purchasing them from a supermarket in Darwin. Therefore, once you’ve bought those items there’s often not a lot left for your fruits and vegetables.”
How and why did HKTC start providing services at the Nightcliff Renal Facility?
“It happened very organically. We had some clients who had to relocate from their Community to Darwin for dialysis treatment, and we assisted them with accessing insurance payments from the superannuation companies. Once we helped those clients other patients, renal social workers and Aboriginal Liaison Officers started asking us to help other people. At that time there was no organisation specifically servicing the renal unit, and some of the patients, while waiting for housing, were staying with family in the town camps, and we were the town camp service provider. So it just made sense to us to fill this gap.”
How many patients do you estimate are at the Nightcliff Renal Facility?
“There are 120. We predominately service patients from Nightcliff Renal Unit but also have a client who is a patient at Palmerston Renal Unit and currently one who is at the Royal Darwin Hospital Renal ward. We have helped about 15 people from the hospital ward.”
What percentage of patients are Indigenous, and where are they from?
“99% are Indigenous, and they come from all over the top end of the NT. We’re currently assisting people who are originally from Wurrumiyanga on Bathurst Island, Minjilang, Yirrkala, Jabiru, Lajamanu, Papunya, Minyeri, Barunga, Borroloola and Galiwin’ku.”
What type of money management and financial counselling does HKTC provide at the renal facility?
“We provide the whole range of services – from helping people do a budget for the change of living arrangements; to accessing ID; through to assisting them to access IP & TPD insurance, debt waivers, advocacy with systemic issues, tax help and delivering information sessions on topics such as understanding their rights and responsibilities as consumers and on affordable lending products such as the NILS loan.”
Are there some issues your team deals with at the renal facility more than others, and what are they?
“Yes, we assist with a lot of superannuation claims and Telstra issues.”
Do you see any health benefits for clients that you’ve assisted, either directly or indirectly, including benefits to mental health?
“There are certainly immediate health benefits for people that we assist, both physically and mentally. How long these benefits last depends on whether there has been a permanent change to their situation, such as stable employment and housing and how much wrap-around support they’re getting from other services. I don’t believe we’ll ever see long-term sustainable change until we can change all aspects of a person’s life that contributes to them being in hardship and ill health to begin with. For this to happen we need to work and keep working collaboratively, from a strengths-based model and programs need to be adequately funded.”
Do you think financial counselling services should become an integral part of health interventions, for example, within health services/hospitals like social work?
“Absolutely. There is definitely a need for impartial and informed free help and advice for people accessing health services, especially when their health needs are going to be long term. We’ve also assisted people, via referrals from Centrelink, who are in hospital receiving treatment for cancer and recovering from an accident. I believe there’d be enough work for a financial counsellor and capability worker to work from the hospital at least one day a week, and this support would take some stress off the patients and their families and free up social workers who would otherwise (and currently are) assisting them.”
Thank you Toni for providing us with some insight into the inspiring work HTKC and yourself are doing to address the socioeconomic issues of patients. You are improving health outcomes by addressing this critical ‘social determinant of health’. We look forward to following you on this journey.
Related research: Indicators of socioeconomic inequalities in cardiovascular disease, diabetes and chronic kidney disease